 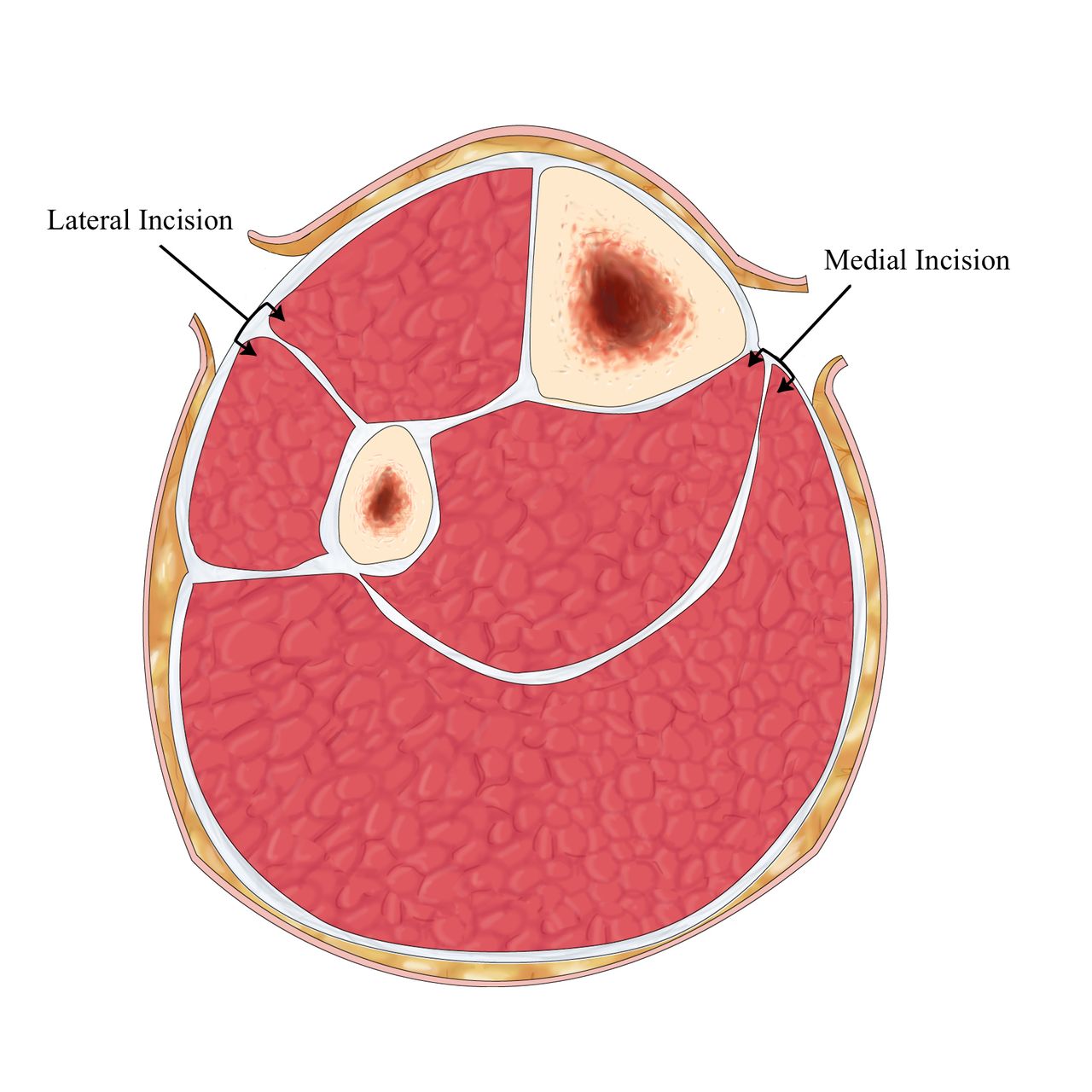 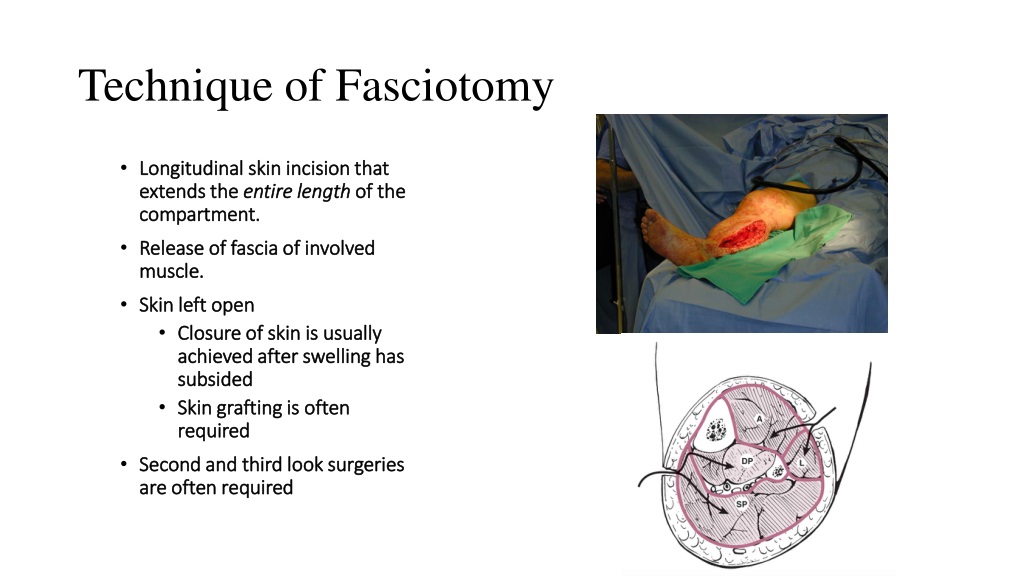
Furthermore, 19 patients requiring muscle debridement, 5 of which were due to incomplete fasciotomies. Major complications (Figure 2) included 7 deaths, (all from associated multisystem trauma) 5 amputations, 5 iatrogenic superficial peroneal nerve injuries. (Figure 1), with 36 (46%) considered major and 15 (19%) minor. Overall, 51 (65%) patients developed complications. The examination demonstrated fractures in 57 (68.7%) patients, and associated vascular injuries in 32 (38.6%) of the cohort. Of note, mean GCS was 12.5 indicating that many patients were not able to fully cooperate for physical examination. Seventy-seven patients critically ill patients over 7 years underwent lower extremity fasciotomy using the double incision technique. The associated complications were divided into major (death, amputation, major muscle necrosis), and minor (wound issues from cellulitis to dehiscence necessitating delayed primary closure, skin grafting, and/or wound vac placement). The method used for fasciotomy was documented, as well as the techniques of wound management till closure. Issues evaluated in the diagnosis and treatment of compartment syndrome included injury pattern, whether fractures were present, associated vascular injuries, time from injury to diagnosis, documentation and frequency of compartment pressure measures, and technique of compartment pressure measurements. Variables evaluated included patient demographics (age, sex), ISS (Injury Severity Score), GCS (Glasgow coma score), as well as surgical intensive care unit and hospital length of stay. All patients who developed lower extremity compartment syndrome during the course of their hospitalization in the presence of multi-system polytrauma were included. Accordingly, we hypothesized that delayed diagnosis and limb loss in lower extremity compartment syndrome was potentially preventable and sought to develop a management algorithm to improve our results.Īfter appropriate IRB approval, a retrospective 7 year review of our prospective trauma database for lower extremity compartment syndrome was performed. Lastly, the current acute care surgery paradigm suggests that the surgical hospitalist will likely be called upon to identify patients at risk for LECS and consequently must have an accurate management plan and be prepared for prompt surgical decompression when necessary.Ī routine audit of the trauma data base at our Level 1 academic trauma center disclosed significant delays in diagnosis and treatment of LECS despite a multidisciplinary team of acute care specialists, including 6 trauma-acute care surgeons, 4 orthopedic trauma surgeons and a trauma- acute care surgery fellow. Additionally, the absence of lower extremity fractures may further reduce the index of suspicion and appreciation of subtle changes in compartment pressures. Furthermore, associated head injury with depressed level of consciousness may significantly compromise the clinical examination and correlation with compartment pressure measurements. 
In addition, a thorough knowledge of regional anatomy is essential to avoid technical morbidity.Įstablishing the diagnosis of lower extremity compartment syndrome (LECS) by physical examination in the multisystem injured patient is often difficult due to the presence of distracting injuries that often require urgent attention. These data underscore the importance of routine surveillance for LECS. In the multisystem injured patient, LECS remains a major diagnostic and treatment challenge with significant risks of limb loss as well as complications from decompressive fasciotomy. Furthermore, 6 patients (7%) had superficial peroneal nerve transections as complications of their fasciotomy. 
Of note, none of these patients had prior compartment pressure measurements. In 7 patients (8.4%), a delayed compartment release resulted in muscle necrosis requiring multiple debridements, subsequent wound closure problems, and long term disability. Fractures occurred in 68.7% (n = 57), and vascular injuries were present in 38.6% (n = 32). ResultsĮighty-three (10 female, 73 male) cases were reviewed. Variables reviewed included demographics, injury patterns, tissue necrosis, amputation and mortality. We performed a prospective review of our trauma registry for all cases of LECS over a 7 year period (2/98–10/2005). Periodic system review of our trauma and orthopedic data for complications of LECS led us to hypothesize that delayed diagnosis and limb loss were potentially preventable events in our trauma center. Despite collaborative trauma and orthopedic management of these difficult cases, significant delays in diagnosis and treatment occur. Prompt diagnosis and decompression of acute lower extremity compartment syndrome (LECS) in the multisystem injured patient is essential to avoid the devastating complications of progressive tissue necrosis and amputation. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
